
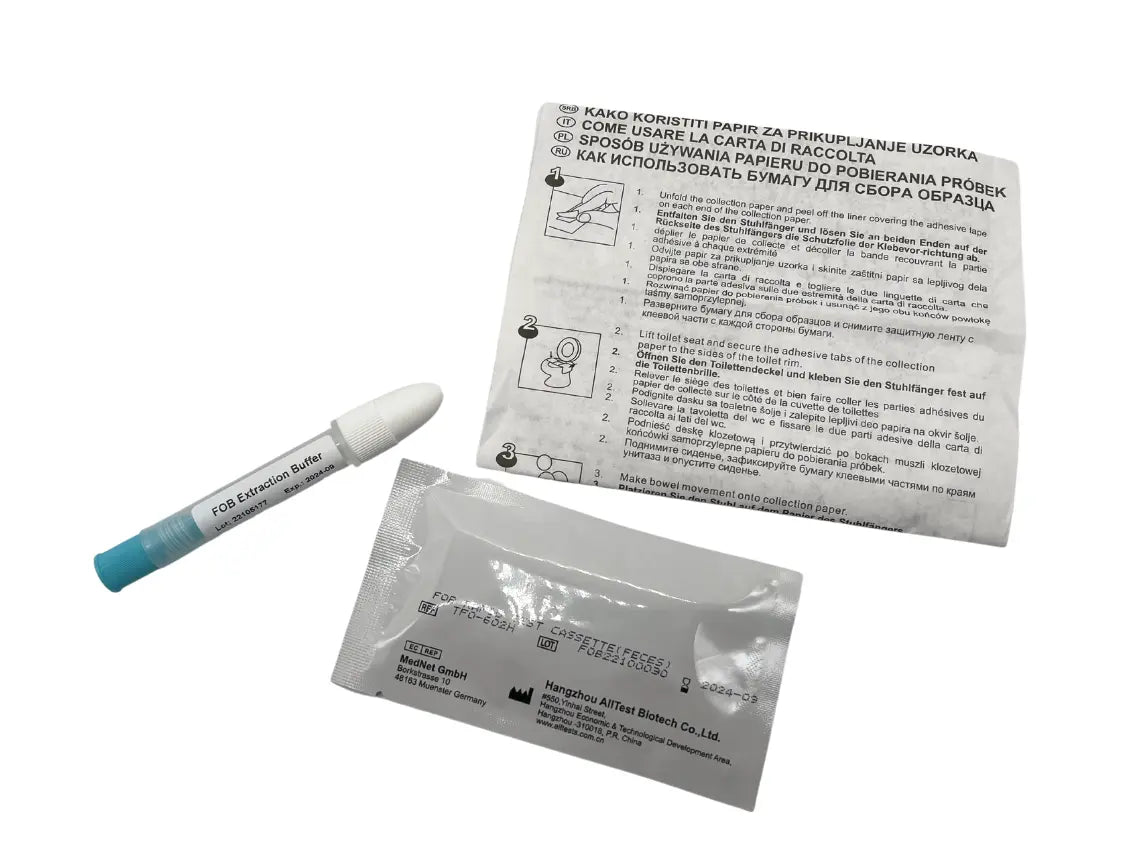
Description
Symptoms

How It Works
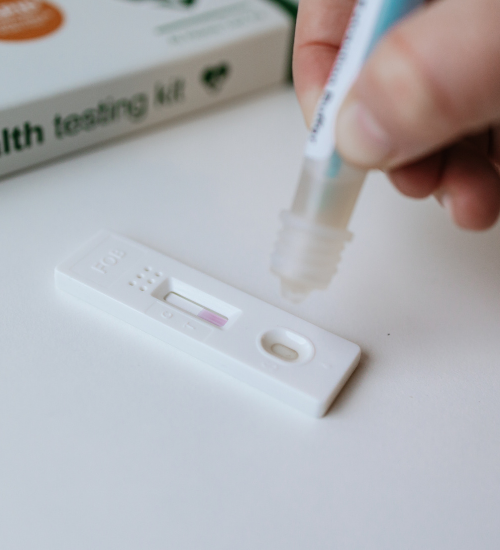
Items Tested
Science
Read more
Read more



